Four overarching themes and several subthemes emerged from the data, all capturing missed opportunities identified by parents of infants with RP. Figure 1 highlights the themes and subthemes.
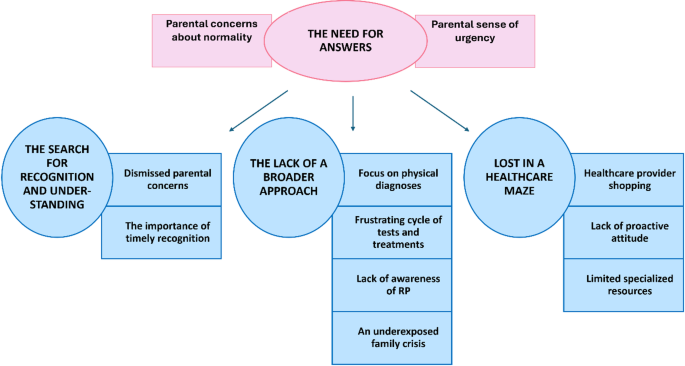
The need for answers
Parental sense of urgency
Many parents reported feeling a pressing need to consult a healthcare provider when their infant experienced, for instance, inconsolable crying. This urgency stemmed from parental uncertainty regarding their infant’s behavior and the potential for serious underlying health issues requiring immediate professional evaluation and intervention. They sought urgent medical consultations, hoping that prompt diagnosis and intervention would quickly ameliorate their infant’s behavior. At that point, the overriding question for parents was: “What’s going on with my child?”.
And I had to go as soon as possible. Because at that moment, you don’t know that it’s going to be something long-term. You know that he cries a lot. And that it’s very extreme. And you think, there is something wrong. And maybe it can be solved. And maybe the pediatrician will see something like, oh, he has this or he has that. I wanted to know. It could be many things. But you don’t realize yet that it’s going to be a child with RP. (Sophia)
Parental concerns about normality
During the interviews, fathers and mothers were asked about behaviors they perceived as atypical, which they now recognize as RP. The responses were diverse, encompassing a broad spectrum, from overextending the limbs or body to being clingy to the parent (see Table 2). Nevertheless, the three most frequently reported RP were crying, sleep disturbances and feeding problems.
Initially, a number of parents believed that their infant’s atypical behavior was temporary and harmless, interpreting it as a result of the early stages of child development. However, over time, many parents changed their minds about interpreting their infant’s behavior as typical. This realization was often triggered by multiple factors, such as the consistent nature of the infant’s behavior, the infant’s increasing age rendering the argument of “growing out of it” no longer viable and the feeling that they had exhausted all possible parental interventions.
At first, you think to yourself, it can’t be perfect all the time, it’s normal, so let’s wait and see, it will get better. But it persisted, day in, day out. We thought, this is really not normal anymore. My wife is also a childminder, for seven or eight years now, and she has helped so many children and parents, including the children with sleep and feeding problems. And those issues got resolved after a while. But not with us. We couldn’t get a handle on our own child. She always said “I can’t do anything more, I have done everything I could and should do”. (James)
A limited number of parents perceived their infant’s behavior as ‘not normal’, ‘different’ or ‘atypical’ from the beginning, even though they were uncertain about the potential cause. For some parents, the primary explanation for this was their contrasting experiences with the older siblings.
We came home and immediately noticed that something was wrong. She cried all day long. We couldn’t do anything to comfort her. We spent the whole day walking around, singing, and trying different things… And then we knew, this isn’t working, this isn’t good for her, this isn’t good for us (Elise).
In some families there was a discrepancy, with mothers expressing greater concern about their infant’s behavior or development compared to fathers, who maintained a more expectant attitude. However, in most cases, both partners shared a similar intuition regarding the behavior of their infant.
My wife has been saying for I don’t know how long, “My child is different”. And I always said “Yes, it will be fine, he will manage well”. “But he can’t talk yet. He can’t speak yet”. “Yes, that will be fine. Einstein also only started talking from the age of four”. So I always see positive things and I always put a positive spin on it. So in that regard, actually, when my wife says or notices something, only then I start looking at it. (Alexander)
The search for recognition and uUnderstanding
Throughout their search for answers, parents expressed feeling disempowered by the tension between their own intuition and the beliefs of others. Despite having a strong feeling that something was wrong with their child, parents’ concerns were often acknowledged (too) late.
Dismissed parental concerns
Parents who voiced their worries about their infant were initially reassured about typical infant behavior. From their family and friends, parents often received dismissive remarks, for example “All babies cry” and “It will get better”. Healthcare providers frequently told parents that the behavior of their infant fell within the normal range of development, such as the peak of infant colic at six weeks of age. They were advised that their infant’s behavior was expected to improve within a few weeks, which in certain cases restored their hope.
I remember that (name of pediatrician) told me at eight weeks, “This is now the peak of the cramps, and hang in there a little longer, in a few weeks it will get better”. (Emma)
Other parents mentioned that the divergence between an infant’s behavior at home versus that in an unfamiliar setting often led them to feel that their concerns were being dismissed. The parents perception was that people in their social network and healthcare providers needed to witness the behaviors firsthand before acknowledging their concerns.
We always noticed that when we went somewhere, she would withdraw into herself, so she didn’t cry much. And the doctor, of course, would get the opposite impression, that she is fine, and she doesn’t cry and she eats well. (Lisa)
Apparently, (name of child) was always very calm at my parents’ house when he stayed over. And because of that, they thought there was nothing wrong. That was difficult for me because then I suddenly came up with (name of IMH clinic) and I got a lot of pushback, but I persevered. I thought, no, this is no way to live. You can all go jump in a lake, but I’m going to do this now for me and my child. Because I feel that this is not okay. (.) And then, there was one evening when I was at my family’s house with (name of child), and he suddenly had a huge tantrum, and everyone got goosebumps. And I said, “This is what I experience every day, all day long!”. So, and… Then finally, there was a little bit of realization. (Isabelle)
Other situations occurred in which parents received unsolicited advice and criticism that was incongruent with their personal beliefs. For many parents, these dismissive responses made them question their intuition and doubt the severity of the situation, often delaying them from seeking (further) professional help.
The advice we got from our family… We did nothing right. “You need to put her in a routine. Then she will sleep”. But that wasn’t the case. (…) We just felt that there was something wrong with her, but we couldn’t understand what it was exactly. And our family didn’t understand that at all. (…) So yes, when did we realize that there was something with her? Actually, from the beginning. But because it was somewhat overshadowed by our family’s judgment and so… we just had to be strong enough to go against that. (Marie)
I have such a good relationship with (name of general practitioner). And yes, now I found it strange that he said, “Come on, you have so much experience, just put him to bed and let him cry, and then he will learn”. And I said, “No, no, it’s not just crying. It’s really screaming his lungs out”. And he said, “Then take him to your sister’s for the weekend, then he will learn that mom is not there, and then he will learn to be quiet”. But I thought, no, that’s not the solution. (…) And I developed such an aversion to the medical field actually. (Evelyn)
A significant number of parents have been subjected to insensitive remarks from healthcare professionals. Parents reported that these comments were deeply hurtful, as they felt a profound sense of misunderstanding from healthcare providers who failed to recognize the immense challenges they were facing at home. Parents agreed that the manner in which information is conveyed significantly impacts interactions. They would have appreciated a more comprehensive understanding of their circumstances.
There was an assistant who made an unfortunate remark in the emergency room: “Are you going to throw your child out of the window or not? No, go home. Yes, then we’ll admit you.” I thought, what is the value of that question? We come because we are seeking help; otherwise, she would already be out of the window, and we wouldn’t need to come anymore. Those are the kinds of remarks… that I really blame. And I consider it a professional mistake. You really shouldn’t make such stupid remarks! (Emily)
We were treated terribly by (name of pediatrician). (Name of child) was crying and arching his back, and I said, “Look!” and the pediatrician said, “Oh, yes, I don’t document those things”. So, she kept saying “You are imagining all those things”. She completely tore us down, and we left feeling very bewildered. (William)
Remarkably, one family noticed that the physician’s viewpoint seemed to shift after the father accompanied the infant to the appointment instead of the mother. The mother, who had consistently felt dismissed when expressing her concerns, believed that the physician had initially attributed the infant’s behavioral issues solely to her parenting. However, observing the infant’s reaction to the father seemed to offer the physician a broader perspective on the factors contributing to the infant’s behavior. The altered perspective led the physician to refer the family to the IMH clinic following a single consultation with the father, in contrast to the multiple consultations with the mother that resulted in no such referral.
So back to that one pediatrician nearby, where I had already been many times. And I felt that he always thought that I was the mom who spoiled my child too much, not letting go properly. But my husband was there with (name of child), who was sick, because I had gone to work. And the pediatrician saw how (name of child) reacted when my husband had to undress him for the examination. How loud he was screaming during that doctor’s examination and so on. (…) I think that then… he thought “Well, this is with the dad, and with the dad, the child also behaves like this, I haven’t seen many babies screaming so loud just to get dressed again”. (Emma)
Overall, almost all parents encountered challenges in communicating their parental concerns, leading to feelings of misunderstanding and disbelief. As a result, they often felt compelled to advocate forcefully for their concerns to be acknowledged.
So indeed, you are constantly in that mode of “We should see now that it’s serious”, but we also have to be able to convey it. So those healthcare providers were always a few steps behind how we experienced it. (George)
The importance of timely recognition
Parents highlighted that it would have saved them a lot of energy and stress if they had been taken seriously from the beginning, instead of having to constantly argue, search for information and make appointments with several healthcare providers. The absence of recognition and timely referrals to specialized care left parents with a sense of wasted time and energy and a belief that earlier intervention could have been beneficial.
But I do think that if we had been believed from the beginning, things would have been different, because being believed is where it starts. (…) There was a professor of pediatrics who holds the principle that a mother is always right, until proven otherwise. That should be the starting point everywhere. And I can imagine that there are incredibly many children and incredibly many worried parents. But I think everyone deserves the benefit of the doubt. It’s about a small child who is essentially helpless. And the parents are too. Because otherwise, the consequences are enormous. The consequences for both the child and the parents. (Emily)
Some parents expressed the profound impact of being validated by their social surroundings and healthcare providers. The acknowledgment of the atypical nature of their experiences, coupled with the assurance of accessible support, offered a crucial sense of hope, alleviating the pervasive feelings of isolation and misunderstanding that had previously burdened them.
But (name of psychologist), she was the first person to finally bring some recognition. Because we didn’t get that from anyone. Not from family, not from friends, not from the healthcare providers. And then the ball actually started rolling quite quickly. We were able to quickly schedule an appointment at (name of IMH clinic). And it was so nice to have someone acknowledge that what you are going through is… (becomes emotional) not normal. (William)
The lack of a broader approach
Throughout their search for answers, parents highlighted that the focus was almost exclusively on possible physical causes in the infant. Socio-emotional factors in the infant and the well-being of the parent(s) were largely overlooked.
Focus on physical diagnoses
Many parents reported how general practitioners or pediatricians typically first focused on ruling out physical causes for their infant’s symptoms, such as GER or CMPI. In some cases, parents had initiated medical consultation driven by their own suspicion of GER or CMPI. Other parents expressed skepticism regarding the diagnosis. Ultimately, a significant proportion of infants received a diagnosis of GER and/or CMPI, 64% (9 out of 14) and 36% (5 out of 14), respectively.
The first doctor I saw said, “Yes, he just has reflux”. I think the first thing doctors say is reflux. “Just give him medication”. I didn’t do that. Because I didn’t believe in it. There were no signs for it. Not that I don’t believe in medicine. I absolutely do, I believe in it, but that didn’t feel right to me. (Sophia)
The diagnosis of GER and/or CMPI often led to prescriptions for medications like omeprazole or a switch to cow’s milk-free formula. Non-pharmacological interventions were also suggested, such as trying a different bottle and attempting an alternative preparation. Moreover, parents commonly turned to alternative treatments, including osteopathy and sleep coaching. Driven by a sense of desperation, parents were inclined to try any advice given to them, in the hope of effecting some positive behavioral change in their infant. Nevertheless, despite numerous interventions offering only temporary relief or partial solutions, parents perceived that the major issue remained unresolved.
We had a very good general practitioner. She had worked with Growing Up for a long time, so she knows children. She said, “Give omeprazole and in a few days your child will be happy again”. So, omeprazole was the first thing we tried, but the problem wasn’t solved. Then we thought, “Maybe it’s cow’s milk protein intolerance”. So, we started with specialized milks. She responded well at first, but very quickly you could see: that wasn’t it either. (John)
We tried many things. In the end, you would spend money on anything just to have less crying. (Lucy)
Not only healthcare providers, but also web-based medical information, online forums, and the parents’ network attributed the behavior to common medical conditions such as GER and/or CMPI. Indeed, the corresponding recommendations for this did not provide a straightforward solution for the infant’s symptoms. The absence of comparable experiences led parents to feel increasingly isolated and atypical.
And I also looked for those groups, online or something. But I didn’t find anything. Some people might not need that, but I was really looking for similar experiences. And the only thing I read was, “Yes, we changed the milk, and it was instantly better”. Or, “We dealt with the reflux, and we had a different child”. And we were so eagerly waiting for when that different child would arrive (laughs cynically). And then you feel like you don’t relate to anyone. I really felt like we were such an exception. That we didn’t have a normal baby life. (Charlotte)
Upon reflection, many parents were no longer convinced that their infant’s symptoms were attributable to GER or to CMPI (only), even though these conditions were initially considered the most likely explanations.
And then eventually, after dealing with all the physical issues, you end up thinking, “There was never -really!- a solution”. We eventually wondered, “Well, he was eating cheese without any problems, so did he really have a cow’s milk protein intolerance?”. (Thomas)
Frustrating cycle of tests and treatments
Many parents described that tests and treatments were repeated, over and over again, in a frustrating cycle of ‘trial and error’. Parents reported that physicians only focused on finding a medical explanation for the infant’s symptoms. Consistently, parents were reassured that all tests were normal and there was no (other) medical explanation (anymore) for the presenting symptoms in the infant. The healthcare focus on the infant, which indicated ‘nothing wrong’ medically, conflicted with the parents’ experiences as they earnestly sought an explanation for their infant’s behavior.
“Look, she is at a healthy weight, her head circumference is good, she urinates enough, she drinks enough, she breathes well, we don’t see any infection in her blood values, her lungs are good, the ultrasound is good, everything is good, voilà, your child is perfectly healthy”. And yet she cries 18 h a day. Well, that’s just… it doesn’t make sense… Because I think, as a person, you look for a reason. Because then you think, so it must be my fault. Or our fault. We are doing something wrong, we are doing it incorrectly. And that’s really tough, that even emergency doctors and pediatricians say, “There is nothing wrong”. (Henry)
After all medical possibilities were ruled out, parents highlighted the fact that that the healthcare providers were just as confused as they were.
The pediatrician investigated all possible medical issues, but really from the perspective of “We have to find something”. But then there came a point where I said it’s nothing medical anymore. Because all medical issues are covered. And then you saw that she was stuck as well. (Charlotte)
Lack of awareness of RP
Nearly all parents were frustrated that healthcare providers tended to focus primarily on physical symptoms and conditions of an infant’s health, often overlooking issues related to emotional regulation and other non-physical aspects. The majority of parents noted a significant gap in healthcare provider knowledge regarding ‘RP’, including a lack of familiarity with RP itself, its management, and the availability of specialized care at IMH clinics. Indeed, most parents agreed that they had never heard of RP before being referred to a specialized IMH clinic and that it would have been helpful if they had known about the existence and management of RP much earlier.
I feel that caregivers focus a lot on the tangible, so the physical, like, “Oh, he has this, or that, or that”. But indeed, everything related to regulation and everything that happens around it, they might not be aware of, because I think they didn’t even know about (name of IMH clinic). (…) I think there’s just too little known about it. (Thomas)
A significant number of parents recommended incorporating awareness and knowledge of RP into the education of healthcare providers. They emphasized that, while healthcare providers should focus on medical aspects, they must also acknowledge broader issues and be aware of RP to better address the needs of families.
I actually think that this should be included in the education for midwives, pediatricians, and so on. It doesn’t have to be extensive, but just to make them aware that it exists. And how can you refer the right families to this or that service? (…) They can focus solely on the medical aspect for all I care, but they must recognize that there is something more going on over there. I needed that at the time. (William)
In addition, some parents advocated for greater public awareness about the possibility of having an infant with RP, as they contended that it is more prevalent than is commonly perceived. They argued that more awareness would enable earlier identification of the condition and expedite access to relevant support services and interventions.
But that’s more of a societal problem. I think it would be good if people who want to have children just knew that, it is an option, a baby with RP. That sounds really strange now, because everyone knows in essence what it is and that it exists. But it seems so unusual. And I realized that it’s actually not that unusual at all. (…) Yes, everyone has that idea. It’s maybe normal that when you get pregnant, you have this imaginary child. And you imagine all sorts of things about it. A bit in a kind of naive optimism or something. I think that’s also good. Because you can’t really start preparing for the worst… that’s such a pessimistic approach. That’s also not something I wish for pregnant people, certainly not. But so, I don’t know. That maybe it should be talked about more… (Audrey).
An underexposed family crisis
Exhausted by the significant strain of the search for help for their infant and the constant medical appointments centered around their infant, parents indicated that they became oblivious to the toll the whole situation was taking on themselves. They recognized that they were experiencing an overwhelming level of stress that significantly compromised their cognitive functioning, hindering their ability to accurately perceive and process information. Consequently, they might have overlooked or misunderstood offers of help or advice, no matter how well-intended. Hence, parents emphasized the importance of timely intervention to prevent them from becoming so overwhelmed that recovery became prolonged.
I was in such a total stress mode at that time that very little really got through. I think that even if there had been someone who understood what I needed and wanted to offer it to me, I might not have been able to accept it or understand what they actually meant. (…) So what did I need at that time? Probably someone who could have prevented me from going so far into the red, because I was so far in the red that it took a long time for my brain to have space again to think differently, to look at myself and my children with some distance. That just wasn’t possible. So I think the main point is that, if parents don’t get the kind of help they actually need in time, even if they don’t know what they actually need themselves, they get so far off track that it takes a lot of time just to bring them back to a place where they are receptive to therapy. (Claire)
However, certain parents pointed out that a singular focus on parental mental health would neglect the broader needs of the infant and the dynamics of both the parent-infant and parent-parent relationships. Hence, an approach that considers and addresses both infant behavior and parental well-being could better identify at-risk families, thereby allowing a timely provision of specialized care.
When we went to (name of center for mental health care) for a month, they said, “Both issues are beyond our expertise, we think you need more specialized help, especially for (name of child). We can guide you as a couple and as parents and help with your concerns, but we also see that (name of child) is exceptionally restless”. They thought it would be better if we moved on to (name of IMH clinic). (…) There, the focus was indeed much more on (name of child). (Lily)
Overall, parents expected that healthcare providers would not merely attend to their infant, but that they would actively engage in further questioning about the well-being of parents, including their emotional state, coping strategies and support networks. Several parents expressed a desire to address the domestic crisis with their healthcare provider, however, they felt that the short routine appointments did not provide adequate opportunities to discuss these matters. According to some parents, Growing Up could play a pivotal role, particularly because they focus on both the individual infant and the family unit, reach nearly all families in Flanders, and provide free, repeated consultations.
What would I want to tell caregivers? That they need to ask more questions and pay less attention to the symptoms, but keep looking at the bigger picture. How is it in that family? How is the stress on that family? How is the connection between those parents and that child? Look much, much further than the symptoms people come in with. And don’t fall into tips and tricks like “Just rub her forehead, then she’ll sleep” (laughs cynically). But really look comprehensively at what is actually going on underneath. That’s what I would say. A child that doesn’t eat. What’s behind that? There’s much more behind it than they assume. (…) Yes, besides the medical AND psychological aspects, of course. And especially the parent-child connection. If the parent isn’t doing well, the child isn’t doing well either, and vice versa. And they need to be aware of that. (Marie)
Lost in a healthcare maze
Throughout their search for answers, parents encountered significant difficulties in identifying appropriate sources of support. Incohesive care provision and the lack of proactivity from healthcare providers complicated parents’ efforts to seek help.
Healthcare provider shopping
Driven by a desire to find an explanation for their infant’s behavior, parents consulted a broad range of professionals, as evidenced in Table 3. A significant proportion of parents primarily sought advice from general practitioners and pediatricians, with a substantial number also consulting Growing Up, osteopaths and midwives. It is noteworthy that no parent mentioned having sought the expertise of a child psychiatrist and only one parent mentioned a child psychologist before the admission to the IMH clinic.
First an osteopath, then clinic after clinic. And then specialist after specialist. (…) I knew there was something. And we saw many specialists to find something. Which led to nothing… (Olivia).
For some parents, even a few days could seem like an eternity, as they were trapped in a domestic crisis. Consequently, certain parents found themselves unable to access timely medical care due to extended waiting lists and turned to emergency departments (20% of the fathers and 33% of the mothers; see Table 3) as a last and only resort when they felt overwhelmed by their infant’s behavior.
In the past, you would go to the pediatrician. Now you have to wait three weeks for an appointment. I find that incredibly frustrating. So you can’t really get medical help unless you go through the emergency room. (…) So the fact that you already hit a wall there, I found that really difficult. Because the emergency room is suddenly such a bigger hurdle to overcome. (Henry)
Conflicting opinions and advice as a result of seeking advice from different healthcare providers left parents feeling directionless. This overwhelmed parents, creating a growing disconnect from their own parental intuition and their infant’s emotional needs. This prolonged uncertainty often led to a decline of trust in the medical establishment and feelings of despair and hopelessness among many parents.
The midwife said, “That tongue-tie is borderline. It can be lasered, but I’m not sure”. Then I went to the baby speech therapist, and she said, “In my opinion, it should be done”. Then I asked an osteopath, but he said, “Can she drink properly at the breast, is milk coming out of her mouth?” I said, “No, it’s not”. And he also said, “Then it doesn’t need to be done”. And someone else said it should be done. And I was like, really, I don’t know what to do anymore. (Evelyn)
A small number of parents expressed that their experience with a previous child had equipped them with the knowledge of how to navigate the healthcare system, allowing them to receive help earlier.
So it’s actually because we had to wait so long with the eldest that we are now quicker with the youngest, because the pediatrician knew about the issues, the psychologist, my psychiatrist… Well, everyone knew about the issues in our family, so we got in everywhere faster. (…) Before you get to the right help, you have to speak to the right person… It’s difficult to get the right help. Once you’re in that whirlwind like with the eldest, then you get to the right help. (Anna)
Lack of proactive attitude
Parents emphasized that they did not expect healthcare providers to solve all their problems immediately, but rather that they acknowledge that they had reached the limits of their expertise, instead of persisting in their own diagnostic and therapeutic approach. Numerous parents experienced a lack of initiative from healthcare providers when considering what might be wrong and proposing possible interventions. Some parents expressed surprise and disappointment at the lack of timely referrals to services that could be helpful for the families. This delayed or absent referral left some parents feeling abandoned by their healthcare providers and seemed to prevent them from efficiently navigating the healthcare system.
I find it quite remarkable overall. Again, there are many people who have done a lot for us and meant a lot to us. But from the general practitioner to the pediatrician to the nutrition team, to neonatology,… No one, no one had the reflex to say “This is trauma and you need to go to child psychiatry”. (Patrick)
Parents eventually ended up at specialized tertiary care IMH clinics in various ways, but nearly all parents reported experiencing a delayed referral. Four families were referred by their pediatrician, three by Growing Up, two by their general practitioner, one by a center for mental health care, one by an adult psychologist and one by an emergency nurse. Remarkably, two families identified the IMH clinic through their own initiative (via a podcast and a television program) and found themselves advocating for a referral, having to persuade healthcare providers who were unfamiliar with the IMH clinics.
They said that you can’t register yourself at (name of IMH clinic). And then it was like, oh, here we go again. “You need a doctor for that”. And then I asked at Growing Up. And they said they can’t do the referrals. And then you’re like, okay, yes, then the general practitioner or the pediatrician. They don’t know about it. So you have to convince them yourself: please help me! (laughs cynically). (Charlotte)
Many parents emphasized the importance of healthcare professionals adopting a more proactive approach and more active collaboration and communication. According to parents, this could facilitate continuity of care and individualized referrals aligned with the unique needs of each family.
Limited specialized resources
Upon first hearing about the concept of IMH clinics, some parents approached it with a degree of skepticism, uncertain about what to expect from the clinic and considering it as yet another avenue to explore. Other parents were eager to explore the potential benefits of an IMH clinic, considering it to be the most appropriate response to their needs. Nevertheless, parents encountered a variable waiting period prior to their admission to the IMH clinic, with an average duration of nearly 10 weeks (see Table 1). A significant number of parents described that waiting period as ‘suffering and surviving’, expressing a desperate need for immediate intervention after exhausting all other available options. Hence, parents emphasized the need for bridging support until the treatment at the clinic could start.
We had our intake at (name of IMH clinic), but then we had to wait a long time before we knew we could actually start at (name of IMH clinic). I think that was especially frustrating because they had indicated that (name of child) would really be in the right place there. But when we couldn’t start right away and the problems persisted… yes, that was frustrating. It was also extra frustrating for us when we were at (name of IMH clinic) and suddenly babies of 2–3 months old were allowed to start. And we had to wait another 6 months while (name of child) was already much older. (David)
A number of parents acknowledged that the extended waiting lists highlight the scarcity of IMH clinics available to provide support for families in Flanders.
That couldn’t go fast enough for me, because there was still a waiting period until a spot became available. I was really hoping every day for a phone call. That happened quite quickly and we are very grateful for that, because we heard from other parents who had to wait longer. This proves that there should actually be many more spots like this available throughout Flanders! (Audrey)
More generally, several parents perceived the mental health services in Belgium to be inadequate. Consequently, parents experienced a profound sense of helplessness and despair, especially when their requests for help were ignored.
There are just few options. Not only for children, but also for adults. Psychological care is just a disaster in Belgium. And there are only a few people who take you seriously. I have often thought, I can understand why some mothers harm their children. If you really say it and you ask for help, and still, no one wants to do anything. Then I can imagine that some parents don’t realize that what they are doing is not okay. That things happen that shouldn’t. Also, it’s sad to see, because I have worked in care myself. (Lucy)
link